Hospitals are trying to control violence. They could prevent it instead
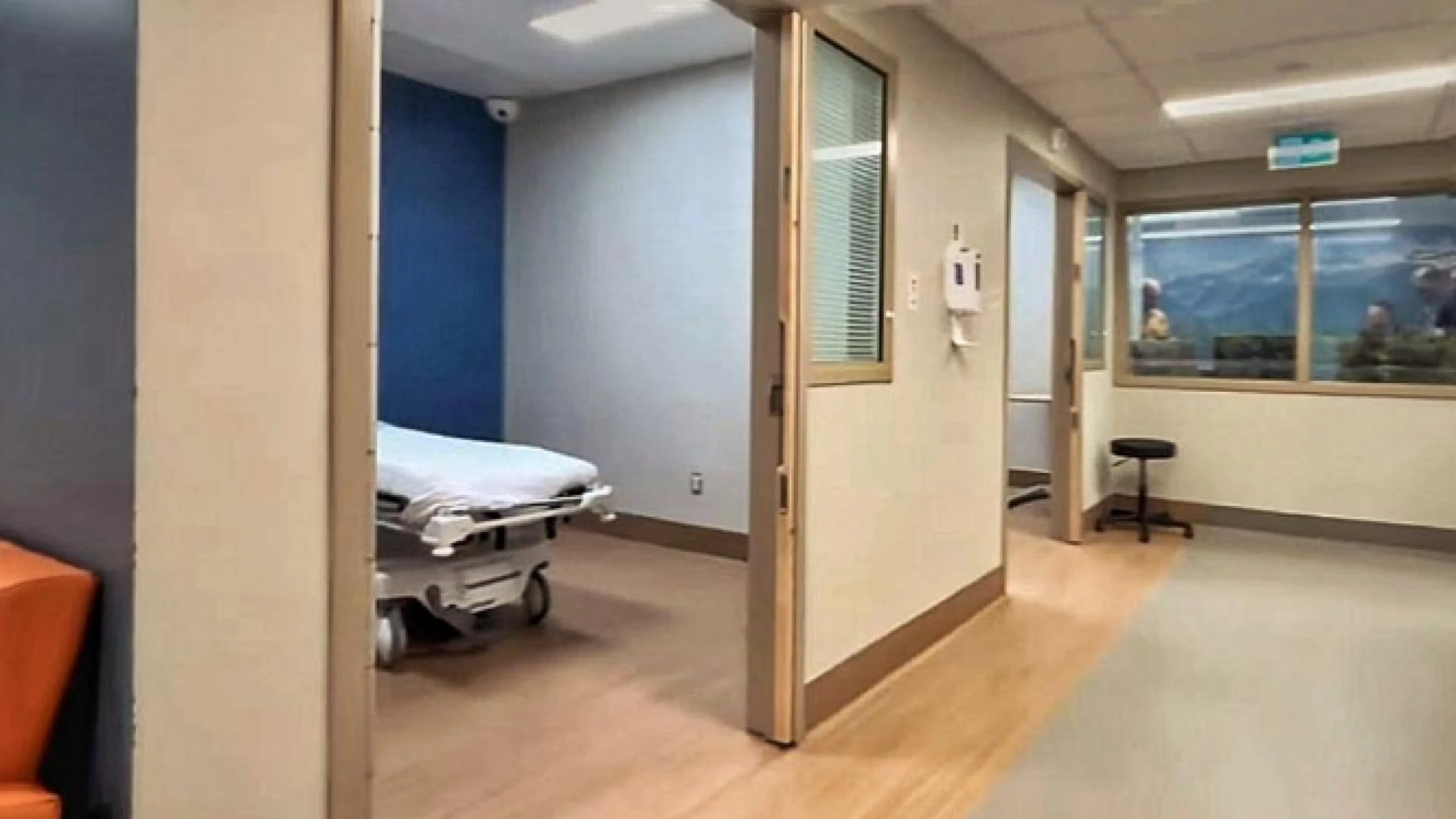
The space is open and bright, daylight filters through the windows. The flooring mimics wood. The colours are calming and the layout supports both privacy and a sense of shared space. Welcome to Montfort Hospital’s emergency mental health zone in Ottawa.
Winnipeg’s Health Sciences Centre paints a sharp contrast. There, very few entrances remain open. Upon entering, visitors must move through turnstiles and are greeted by security guards. Once inside, police patrol the corridors and AI-powered weapons scanners adorn both the adult and pediatric emergency rooms.
These disparate environments represent two very different approaches to addressing safety in hospitals.
Despite the rapid expansion of security measures in hospitals across Canada, there is no available data showing that they concretely improve safety outcomes.
A 2022 article in The Hastings Center Report describes a different school of thought to managing increased safety concerns in hospitals. It argues that the design of health care spaces influences behaviour and emotional states.
“...we in the medical, bioethical, and public health professions know that the built environment has profound effects on those within a space,” write the article's four authors, a multidisciplinary team spanning medicine, architecture, and bioethics.
Policing, by design, responds to violence after it has already occurred. It introduces surveillance, scrutiny, and an explicit assumption that patients and visitors are potential threats.
The Hastings authors propose that most hospital leaders underestimate the impact physical design of their facilities has on patients, both positive and negative.
Violence in health care is not a marginal issue. A recent cross-country survey of nurses found that 95 per cent of them experienced some form of violence or harassment in the past year. Nursing organizations describe a worsening national crisis and report increases in violence-related injuries across multiple provinces.
Nursing unions, such as the Manitoba Nurses Union, have voted to grey-list certain hospitals, among them, the Health Sciences Centre, which means nurses are advised not to seek employment there.
Lisa Streeter, a Clinical Nurse Specialist in Winnipeg, says safety is a two-way street. Violence can be directed at staff or patients.
“It is also about patients and families feeling safe in accessing the care that we provide” she says. “I feel that the idea of safety is bigger than just reducing the risk of physical violence through force. I think that it's really about trying to prevent that escalation right from the start.”
The emergency mental health zone at Montfort Hospital in Ottawa demonstrates this approach. There, the physical environment is seen as an integral part in the care of patients.
The small unit, nested within the emergency department, opened to patients in November 2024. Brightly coloured furniture contrasted by walls painted in tones of blue, warm white and a wall graphic depicting the Rocky Mountains.
Daylight and sightlines to the outdoors contribute to a sense of calm.
“We maximized the number of windows that we could create,” says Cédric du Montier, project architect and senior associate with Parkin Architects, which designed the space.
“We have wall graphics representing scenes of nature,” he says, also noting that the nursing station’s glass barrier is covered in a perforated film. “So, when you are in the patient environment you don’t feel observed.”
A visual connection remains without the sense of surveillance.
The design prioritized both patient and staff well-being, by providing environmental cues to deescalate agitation when necessary.
When we enter a building and are guided to move through a space, it plays a role in how we feel and engage with the people and services provided, says du Montier.
Peter Sampson of Public City Architecture says, “Do people feel a sense of belonging when they come to that space? If you offer something compelling that strikes a sense of awe in people … they will feel appreciated no matter who they are, and they will treat the space and the program and the people who work there with a decent level of respect.”
When asked to imagine an ideal work environment that could aid in making meaningful connections with patients, Streeter describes a space with lots of natural light and references to nature. A space that is quiet and affords some privacy.
In today’s climate, security and enforcement-focused measures are increasingly preferred. But without evidence that these measures improve safety, examples such as Montfort’s emergency mental health zone show another way forward.
—
Nadin Gilroy is a physician and journalist based in Winnipeg with a focus on health equity.