You’re reading the web version of our email briefing on health policy, science and medical news. Sign up to get the next one.
Welcome back Healthwatchers,
This week: Alberta privatizes air, promising improved breathing efficiency.
In a bid to “optimize access to oxygen and streamline the respiratory experience,” the Alberta government announced today its plans to…
Kidding. (Probably.)
It’s April Fools’. But today’s stories are real, even if some feel like they shouldn’t be.
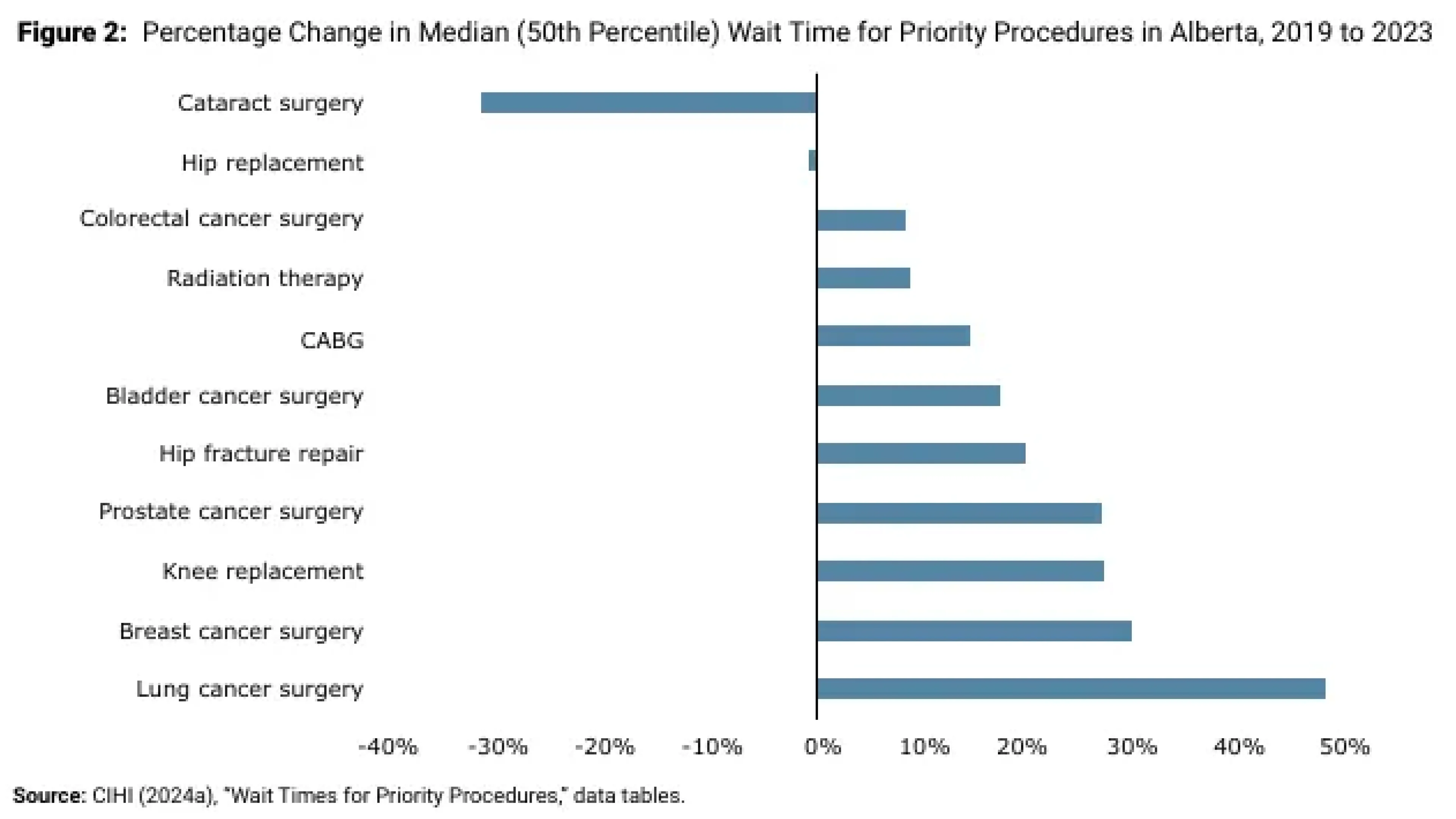
Outsourced surgeries have surged, and so have wait times.
Why it’s important: A new report says Alberta’s push to expand private surgical contracts has diverted scarce staff and funds from the public system, worsening conditions for complex patients. Since 2019, provincial spending on private surgeries has nearly tripled.
Cancer surgeries, which are done only in public hospitals, face longer delays as anesthesiologists and other staff move to higher-paying, simpler work in private clinics. Health Minister Adriana LaGrange dismissed the findings as ideological. But public ORs are sitting idle while resources flow to easier, higher-margin cases.
Read more…

The company’s most valuable asset — genetic data — is up for sale.
Why it’s important: Genetic testing giant 23andMe filed for bankruptcy in the U.S., triggering concerns over what happens to its trove of health data.
The company collapsed after a 2023 breach leaked DNA-linked profiles of nearly 7 million users. Its data, already used by pharma companies for drug-discovery, can now be sold to new buyers for new purposes. While 85 per cent of users agreed to research use, experts say it's unclear how future owners might use the data. California's attorney general encouraged anyone with a profile to delete their data. In Canada, a privacy probe launched last year is ongoing.
Read more…

Not every primary care issue needs a doctor. But public coverage still says otherwise.
Why it’s important: With 6.5 million Canadians lacking a family doctor, some experts say expanding public coverage to nurse practitioners, pharmacists, and other providers could unlock faster access and better care.
Alykhan Abdulla, a family doctor and board director with the College of Family Physicians, says the system clings to a 40-year-old model that funnels all care through MDs. Policy introduced in the waning days of the Trudeau government comes into effect a year from now, treating services by “physician-equivalents” as billable under the Canada Health Act.
Read more…
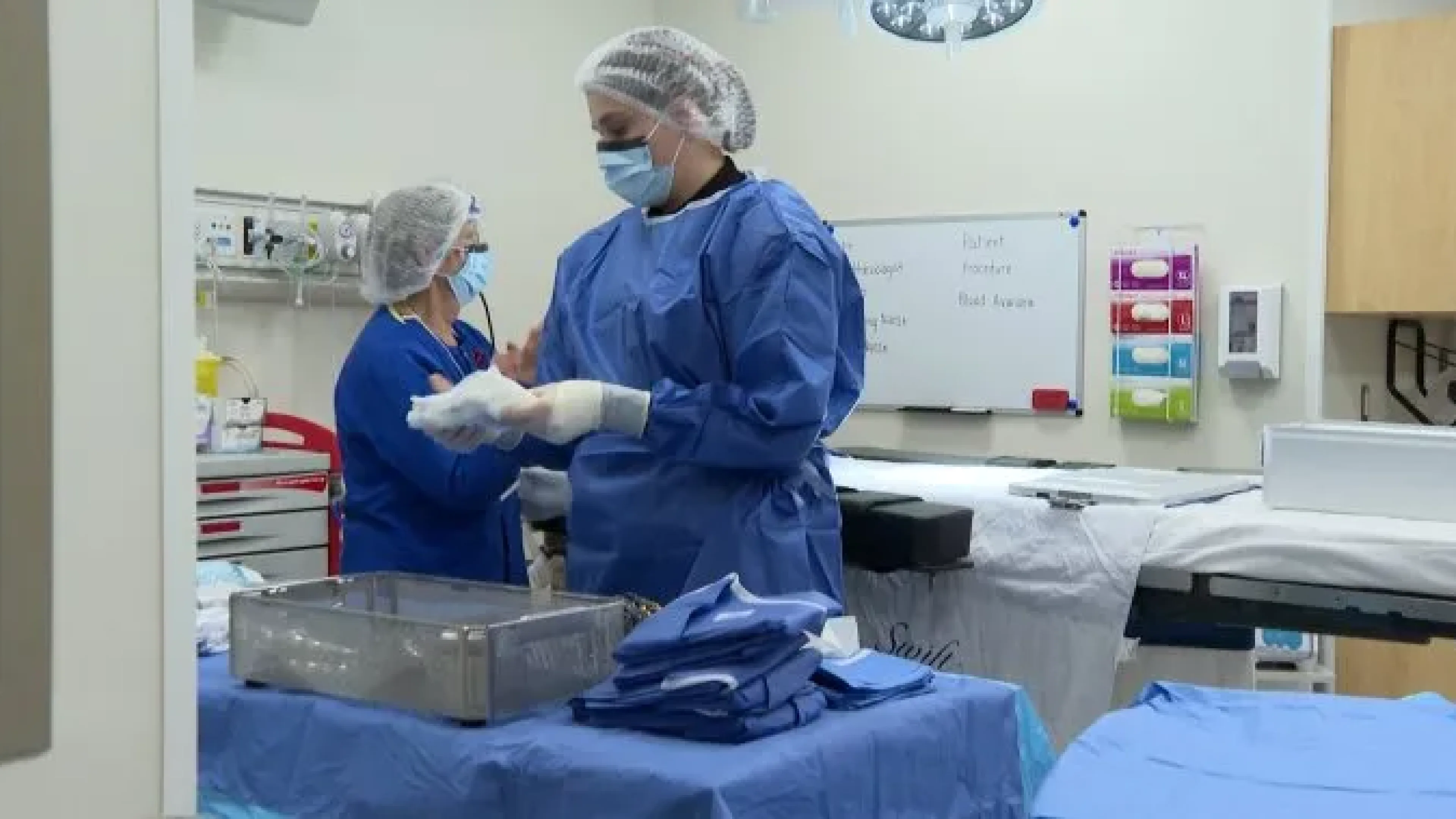
As Ontario asks NPs to save primary healthcare, more than half surveyed say they’re thinking of quitting.
Why it’s important: With pan-Canadian licensing expected in 2026, the stage is set for a predictable exodus of NPs to higher-paying provinces. Ontario NPs in publicly-funded clinics earn about 25 per cent less than their counterparts in B.C.
In a survey of 437 NPs, few reported being being “very satisfied” at work — just over 12 per cent. Advocates blame underfunding, low pay, and a lack of support, even as workload expectations sharply rise. “We’re doing much more with less,” says NP Aliya Hajee. She says NPs aren’t just supporting the system, but helping to hold it together.
Read more…

Sudden, sweeping layoffs at U.S. health agencies devastate disease surveillance and outbreak response — posing clear risks to Canada.
Why it’s important: Speaking at the bi-annual Canadian Medical Association summit, former CDC director Dr. Tom Frieden singled out measles, pertussis, and drug-resistant TB as major threats. “It may take time to see the damage,” he said, “but it’s really quite substantial.”
Frieden said the U.S. had a history of neglecting francophone countries in Africa with its foreign aid efforts, and that Canada could be very helpful in this respect. Senior New York Times health reporter Apoorva Mandavilli, who also spoke, said the gutting of domestic HIV-prevention efforts in the U.S. will affect Canada.
Read more…
“Patients come in and they just talk to you, about doctor things. That’s a profound relief.”
Why it’s important: This firsthand account by a U.S. emergency physician now practicing in B.C. has struck a chord with patients and providers alike. Since we published it, it’s been widely shared by Canadians who recognize themselves in his reflections, and in what he left behind.
The piece explores how “defensive medicine” distorts care in the U.S., and how trust between doctors, patients, and the systems of which they are a part shapes the work. “Canadian doctors care for their fellow citizens in a system designed — however imperfectly — for the public good,” he writes. “That idea still holds power.”
Read more…
That’s it from me.
One thing that stuck with me this week: just how blunt Tom Frieden and Apoorva Mandavilli were about the global fallout from the U.S. DOGE cuts, and the direct risk to Canada.
Also, that nurse practitioner burnout survey — I knew it was bad, but not that bad.
I hope you enjoyed this April Fools’ edition. Back next week with more.
No pranks, promise. 🤞
Nick Tsergas, Editor
Canada Healthwatch
[email protected] | canadahealthwatch.ca
Stay informed.
On the most important developments in Canadian health.
Get Canada’s essential briefing on health policy, science, and system change. Get Briefing